Approximately 68.8% of US adults are overweight or obese*
*According to data collected from the United States National Health and Nutrition Examination Survey.
86 million Americans are considered pre-diabetic*
*Which means they are at risk of developing diabetes within 3-5 years, (90% of them don’t know it).
Additionally, a large burden of health care costs can be attributed directly to obesity as well as multiple, potentially preventable, comorbidities such as cancer, cardiovascular disease, and diabetes. As a result, national organizations, such as the US Centers for Disease Control and World Health Organization, have made halting the rise of the obesity high priority.
Pharmacists play pivotal role in diabetes prevention, initiating weight loss, and halting obesity
Pharmacists, commonly considered the most trustworthy and accessible health care professionals, are ideally situated to identify those at risk, start a dialog regarding prevention and refer patients to Lindora for a weight loss and wellness program.
Educate patients about the benefits of weight reduction
US Pharmacists role and the evidence
Pharmacists can have a positive effect on patient health by educating patients about the benefits of even modest weight reduction. In one study, patients who were told they were overweight by a health care professional were 88% more likely to lose 5% of their initial weight than patients who were not alerted to the weight problem.6 It is important for pharmacists to educate patients that obesity is a disease state and that it is associated with several comorbidities and an increased risk of cardiovascular events.1-5 Patients should be aware that a modest reduction in weight (3% to 5% of initial body weight) may have a clinically meaningful effect on cardiovascular risk factors… 1 Pharmacists interact with patients with obesity-related comorbidities (eg, hypertension, type 2 diabetes, dyslipidemia) on a daily basis and can help identify those who would potentially benefit from more intensive weight-loss interventions. Based on guidelines for the management of overweight and obesity, pharmacists can direct patients to seek medical care when appropriate and provide counseling on options for weight reduction, including lifestyle modification and pharmacotherapy.”
Weight loss has been shown to lower blood pressure and blood sugar, and improve lipid levels. Research also shows that improving the health risk profile reduces healthcare costs and may improve productivity.
Weight loss programs that have the best outcomes are those that assist individuals in making necessary and sustainable modifications to their eating and exercise habits through medical supervision, individual diet modification, and frequent interaction with a medical professional .
Data also suggests that to maintain long-term weight loss it is critical for care providers to understand and address the underlying psychological issues that accompany obesity, and to develop a “therapeutic bond” to assist the patient as they modify their behavior and choices.
Overview of the Lindora Clinic Program
The Lindora program is a medically based, proprietary weight loss and weight management program. The program and protocols has evolved since 1971 through continuous patient treatments within a specialty medical practice. It is built upon a multi-faceted physiological, behavioral and cognitive therapeutic lifestyle change approach to promote long-term results.
It provides a personalized program that addresses each aspect of the patient’s core lifestyle (e.g., nutrition, physical, psychological, social support and stress management). The program has two main phases: weight loss and lifetime maintenance.
 Weight Loss Phase
Weight Loss Phase
The weight loss phase utilizes a reduced calorie diet which facilitates converting the body’s stored fat to energy. Daily menus consist of lean proteins and fruits and vegetables, as well as small protein based snacks. During this phase, the patient visits the clinic multiple times per week to meet one-on-one with a licensed nurse or health educator that has extensive knowledge of the Lean for Life program to review their Daily Action Plan and Food Diary; record their weight; discuss their “plan of action” for any anticipated challenges; develop strategies for addressing those challenges. The frequent short visit modality supports and reinforces the behavior change process. These daily visits take 5-7 minutes. During each visit the requisite therapeutic bond with the clinician is established, providing the patient with accountability required for their success.
Lifetime Maintenance Phase
The Lifetime Maintenance phase is structured to reinforce the healthy habits that are necessary to maintain the achieved weight loss results. This unique component of the Lean for Life program is the core upon which the patient’s long-term success is built.During this phase patients continue to visit the clinic regularly, but less frequently. This structure provides the continued accountability that reinforces lifestyle changes. If necessary, a brief “refresher” weight loss program can be recommended.
The Lindora Clinic Patient Experience
The Initial Contact
This is an introductory visit. During this visit the prospective patient will meet with a program expert (Lindora Clinic trained nurse, provider, or health educator). An evaluation will be made based on weight, medications, BMI and Lindora’s proprietary health risk assessment. A few moments will be spent to introduce the Lindora weight management program and the health benefits of achieving and maintaining a healthy weight. Together the program expert and patient will set goals and create a plan for realizing those goals.
Prior to beginning treatment
Program Visits
The patient is provided verbal and written instructions on how to get started on their Lindora weight loss program. The program model has each patient coming into the clinic multiple times per week during their treatment term. Each treatment session includes routine measures such as: weight, body measurements, blood pressure, pedometer steps/ exercise minutes and a review of the prior daily action plans (DAP) and medication regimen.
The DAP includes: foods eaten, carbohydrate, fat and caloric intake, and amount of fluid and medications consumed. After this assessment new plans are created for the intervening days and individualized behavior modification counseling is provided to each patient. The initial consultation and the physical exam take approximately 20 minutes each. A daily treatment session takes 5-7 minutes.
The Evidence… Lindora Clinic Program Outcomes
Analyses of patients’ weight loss during their first ten-week program are shown below, indicating consistently over 10% weight loss in the program.
Lindora Internal Patient Data and Analysis
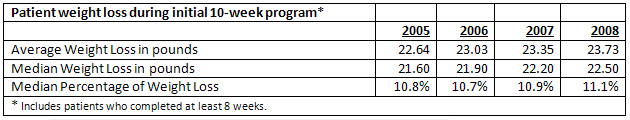
*internal data and analyses
Another study of 584 Blue Cross of California members demonstrated significant improvements in metabolic risk factors after the initial Lindora 10-week weight loss program. Analyses depicted below on the graph show that for patients in the disease zone for indicators including waist circumference, cardiac risk ratio, triglycerides, blood pressure, fasting glucose and BMI all improved (patients were no longer considering in the “disease zone”) at the completion of the LFL program.
Blue Cross of California Member Study
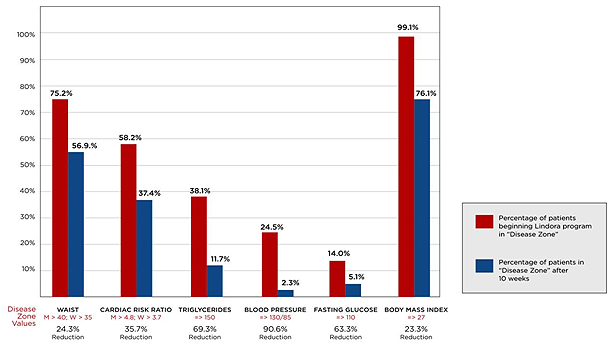
Sustained Outcomes
Depicted below is change from patient’s starting weight at initial program to the most recent weight for patients who presented at a Lindora clinic for a weight check in 2008. The cohort includes all patients who presented in 2008 and had a first weight loss program 5 or more years prior. The data shows that of this cohort 79.07% of patients maintained baseline or lower weight levels. It also demonstrates that 42% maintained 5% weight loss or greater.
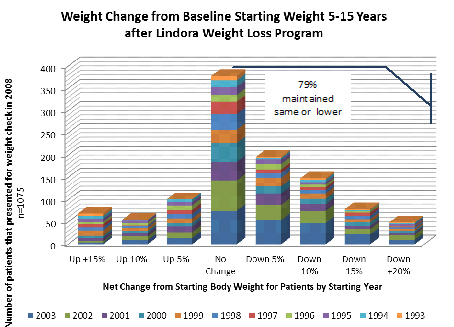
Lindora Clinic and Pharmacy
How pharmacists collaborate with Lindora?
The medically supervised programs developed by Lindora provide the clinical interaction necessary to achieve and maintain significant weight loss. The collaboration across trusted health care clinicians, pharmacists and health coaches is important to influence patient awareness, access and action. 45 years of experience and evidence point to the efficacy of the Lindora program in addressing obesity, diabetes prevention and co-morbidities of obesity including Type 2 Diabetes, cardiovascular disease and hypertension.
Below are two papers deal with pharmaceutical management and weight loss while on the Lindora program that demonstrate value and importance of collaboration with a patients pharmacy team:
- Weight Loss Results After One Year of Continuous Treatments at A Medically Supervised Weight Loss Clinic
- Does Prior Authorization of Sibutramine Improve Medication Compliance or Weight Loss?
Footnotes
- 1. Jensen MD, Ryan DH, Apovian CM, et al; American College of Cardiology/American Heart Association Task Force on Practice Guidelines; Obesity Society. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society.J Am Coll Cardiol. 2014;63(25 Pt B):2985-3023. doi: 10.1016/j.jacc.2013.11.004.
- 2. Fryhofer SA. Is obesity a disease? In: Report of the Council on Science and Public Health. Paper presented at: 2012 Annual Meeting of the American Medical Association. CSAPH Report 3-A-13. a13-addendum-refcomm-d.pdf. Accessed April 20, 2015.
- 3. Mechanick JI, Garber AJ, Handelsman Y, Garvey WT. American Association of Clinical Endocrinologists’ position statement on obesity and obesity medicine. Endocr Pract. 2012;18(5):642-648. doi: 10.4158/EP12160.PS.
- 4. Apovian CM, Aronne LJ, Bessesen DH, et al; Endocrine Society. Pharmacological management of obesity: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2015;100(2):342-362. doi: 10.1210/jc.2014-3415.
- 5. Council of the Obesity Society. Obesity as a disease: the Obesity Society Council resolution. Obesity (Silver Spring). 2008;16(6):1151. doi: 10.1038/oby.2008.246.
- 6. Pool AC, Kraschnewski JL, Cover LA, et al. The impact of physician weight discussion on weight loss in US adults. Obes Res Clin Pract. 2014;8(2):e131-e139. doi: 10.1016/j.orcp.2013.03.003.
